What Is Retrocalcaneal Bursitis?
Retrocalcaneal bursitis is a common cause of posterior heel pain, often affecting runners and athletes. Also known as Achilles tendon bursitis or heel bursitis, it occurs when the retrocalcaneal bursa, a small, fluid-filled sac located deep between your Achilles tendon and the calcaneus (heel bone), becomes irritated, swollen and tender. The retrocalcaneal bursa is lined with a thin layer of synovial fluid that normally reduces friction during movement, but repeated compression can cause inflammation, making walking, running and jumping painful.
While it can feel similar to other conditions, such as Achilles tendinitis, Achilles tendinopathy, or plantar fasciitis, retrocalcaneal bursitis is a distinct problem that may require a different treatment approach. A differential diagnosis is important because these related pathologies can occur together, including insertional Achilles tendinopathy.
How to tell the difference:
- Heel Bursitis discomfort often feels more like a sharp pinch when the area is squeezed (like when you bend deeply or wear tight shoes).
- Achilles tendinitis usually feels more like a dull ache or soreness in the tendon itself, especially with high-force activities like jumping or heavy calf exercises.
- Plantar fasciitis causes stabbing discomfort and inflammation of the plantar fascia, the tissue connecting the heel to the toes. It is worse with the first steps after rest, such as in the morning.
It’s helpful to know that there are two bursae in this area. The one causing retrocalcaneal bursitis is the deep subtendinous bursa, situated between the tendon and the bone. A second, superficial subcutaneous bursa (the subcutaneous calcaneal bursa) lies between the skin and the tendon and is more often irritated by footwear rubbing. Identifying the correct bursa is important because the causes and treatment plans are not always the same.
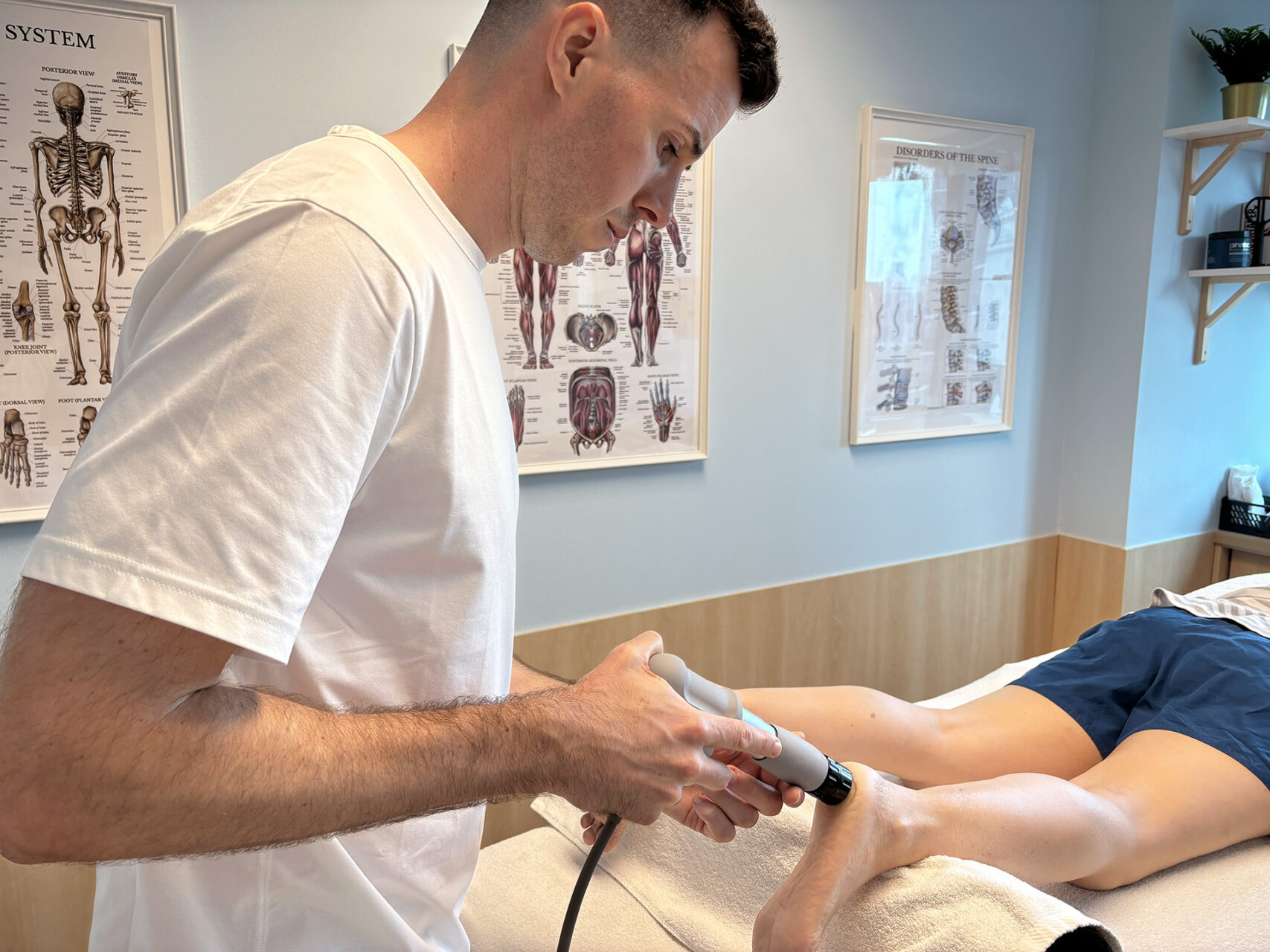
Retrocalcaneal Bursitis Causes
Retrocalcaneal bursitis is caused by factors that mechanically irritate the fluid-filled sac (bursa) at the back of your heel. This usually occurs when the retrocalcaneal bursa is pressed between your Achilles tendon and the anterior surface of your calcaneus, especially when your foot is bent upward (dorsiflexion).
Common causes include:
- Overuse or sudden changes in activity. Activities that involve repeated pushing off and landing, such as running, court sports or dancing, can irritate the bursa due to excessive loading. This is more likely if you increase the amount or intensity of your training, especially on hills.
- Poor-fitting or unsupportive shoes. Footwear can put pressure and cause friction on the back of the heel. Stiff heels, tight-fitting shoes, thin padding, or constant rubbing can aggravate the affected bursa. Wearing high-heeled shoes, very flat shoes, or a sudden change in heel height can also increase strain on the Achilles tendon. High-heeled shoes alter the resting length of the tendon and may contribute to inflammation over time.
- Movement, muscle, and bone issues.
- Tight muscles. Tight calf muscles or limited dorsiflexion can increase pressure at the posterior aspect of the calcaneus when you move.
- Foot shape. Biomechanical abnormalities, such as high arches or feet that roll inward, can alter how force is distributed in the adult foot, increasing local stress.
- Bone shape. A bony prominence on the posterior aspect of the calcaneus (called Haglund deformity, or Haglund’s syndrome) reduces space in the retrocalcaneal recess and increases pressure on the retrocalcaneal bursa and Achilles tendon. Haglund’s syndrome is one of the most common structural causes of retrocalcaneal bursitis.
- Injury. A direct blow or fall on the back of the heel can cause sudden heel swelling and local swelling.
- Underlying health conditions. Diseases such as rheumatoid arthritis, gout and other forms of inflammatory arthritis can cause bursal inflammation.
- Age. The risk can increase as you get older, partly due to normal changes in tendons and tissues, especially in active individuals.
- Infection. In rare cases, the bursa can become infected. This is a serious concern if you notice significant redness, warmth, or fever, or if you feel generally unwell, and it requires immediate medical attention.

Retrocalcaneal Bursitis Symptoms
Catching this condition early is key to keeping a short-term irritation from becoming a lasting problem.
Early retrocalcaneal bursitis symptoms often include:
- Pain and tenderness at the back of the heel that worsen with activity and get better with rest.
- Pain or discomfort when pushing off, walking uphill, climbing stairs, or deeply bending your foot.
- Swelling or a soft, warm bump near where the Achilles tendon connects to the heel.
- Discomfort when wearing closed-back shoes, especially if the heel counter presses on the inflamed area.
- Stiffness after resting, such as in the morning or after sitting for a while.
It can be confusing when symptoms improve after a warm-up, only to return later. If you continue training through theearly irritation, the small fluid-filled sac (bursa) can become more inflamed. Ignoring the inflammation can eventually change the way you walk, potentially leading to strain in your knee, hip, or lower back.
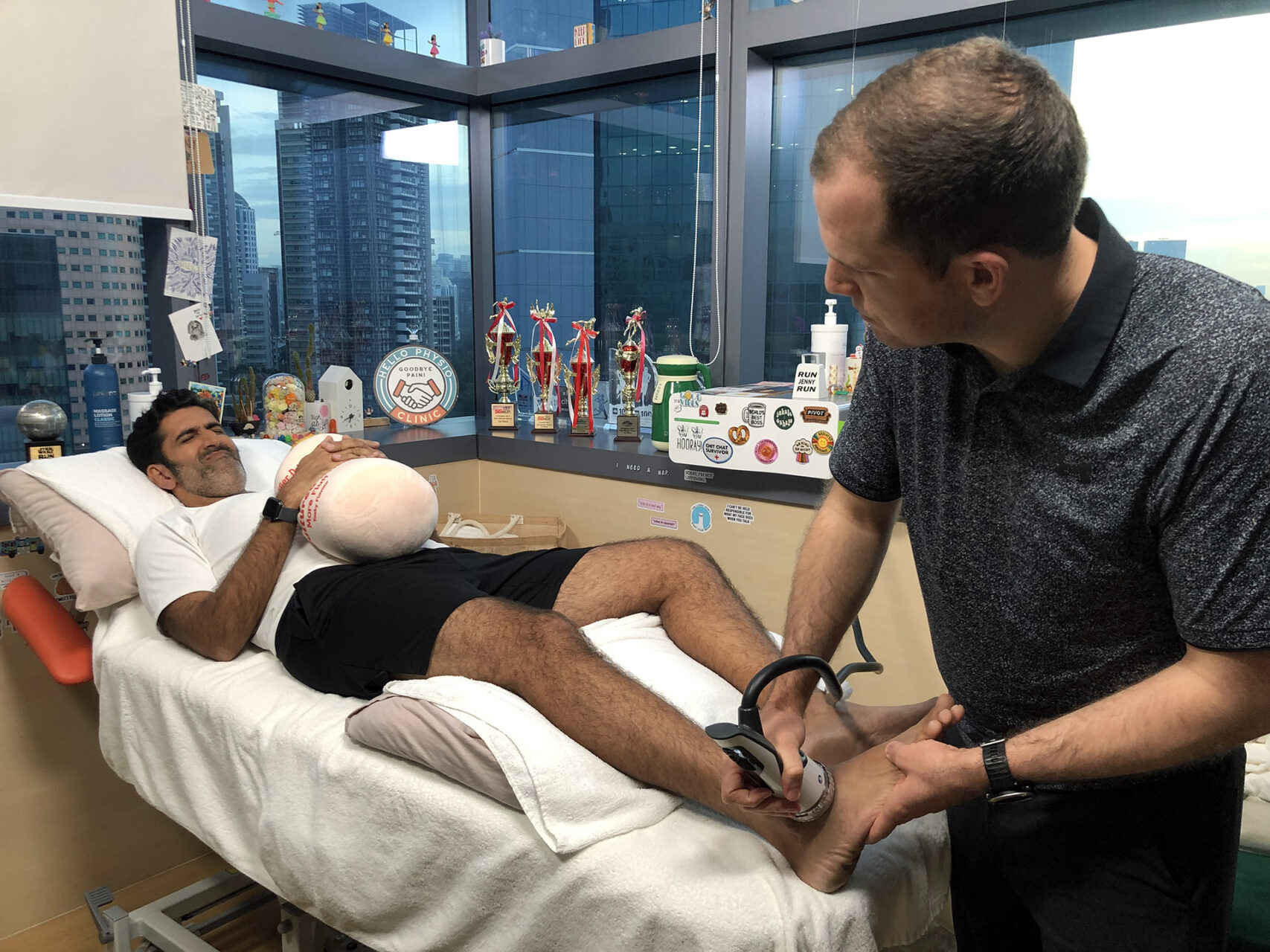
Diagnosis
Diagnosing retrocalcaneal bursitis typically starts with a thorough physical exam and a discussion of your symptoms. Your doctor, physiotherapist, or sports medicine specialist will look for swelling, warmth, and the precise location of your pain. Tenderness that is strongest on the sides of the Achilles tendon insertion (where it meets the heel bone) rather than directly on the tendon suggests the retrocalcaneal structure is the main problem.
The exam also checks for factors that might be causing the irritation, such as a tight calf, limited dorsiflexion (ability to point your foot up), foot structure issues, or how your heel lands when you walk or run. Simple checks, like a single-leg balance test or a controlled heel raise, can help guide treatment. A physical medicine approach considers the full kinetic chain, not just the site of discomfort.
Imaging is not always needed, but may be helpful if:
- Symptoms don’t improve.
- The diagnosis isn’t clear.
- A bony prominence, such as Haglund’s deformity (Haglund’s syndrome), is suspected.
- Retrocalcaneal bursitis ultrasound can demonstrate bursal inflammation, assess whether the affected bursa is swollen, and evaluate the distal Achilles tendon and tendon insertion for damage.
- A weight-bearing lateral radiograph can spot a Haglund’s syndrome bony prominence, lateral expansions of the retrocalcaneal recess, or blunting of the Kager fat pad. However, X-rays alone are not always definitive.
- Magnetic resonance imaging (MRI) provides more detail when a tendon injury, stress fracture, or other cause is suspected. MR imaging findings can help distinguish retrocalcaneal bursitis from tendon pathology.
Getting the correct diagnosis is important because this condition can be mistaken for other types of heel discomfort, and proper treatment depends on the true cause of your symptoms.

Retrocalcaneal Bursitis Treatment
Retrocalcaneal bursitis treatment depends on the severity and the triggers that continue to compress the bursa. Rest can temporarily reduce discomfort, but long-term improvement usually requires proper treatment that addresses the irritant and rebuilds load tolerance.
Retrocalcaneal bursitis home treatment to reduce compression and calm irritation
For mild cases, early conservative treatment focuses on reducing pressure in the posterior area.
- Activity changes. Temporarily reduce hills, speed work, deep squats, and anything that may trigger a sharp pinch at the back of the foot.
- Ice and short-term relief. Ice can help settle soreness. Over-the-counter anti-inflammatory medicines may help some.
- Footwear adjustments. Avoid stiff heel counters and wear shoes that reduce direct pressure. Footwear adjustments are often the single most important early step. A small heel lift or heel pad may temporarily reduce compression.
Restore motion and reduce calf tension
Once the discomfort settles, treatment shifts toward improving mobility so the bursa is not repeatedly squeezed.
- Physical therapy addresses both the local inflammation and the contributing factors.
- Manual therapy can help address calf tightness and joint restrictions that limit motion.
- Dry Needling may be used for stubborn calf trigger points that restrict movement and increase local stress.
- INDIBA® may be added when appropriate to support comfort and circulation in irritated tissues, especially when symptoms limit your ability to start strengthening work.
Reload the calf and Achilles, then return to sport
Strengthening is the long-term anchor for recovery, but it must be done carefully to avoid excessive compression.
- Isometric calf holds can help reduce pain early while keeping the calf engaged.
- Progressive calf strengthening builds tissue capacity and improves push-off mechanics.
- Eccentric heel drops may be useful for some people, but they are not always the first-line treatment for retrocalcaneal bursitis. If deep bending increases pinching, your physiotherapist will modify the range and technique so you can strengthen without repeatedly compressing the bursa.
As symptoms improve, rehab progresses to impact work, jumping, and sport-specific drills to help the heel tolerate real-world demands again.
Adjunctive modalities when symptoms persist
If recovery is slow, modalities may help reduce irritability, allowing strengthening and load management to progress. In severe cases, multiple modalities may be combined.
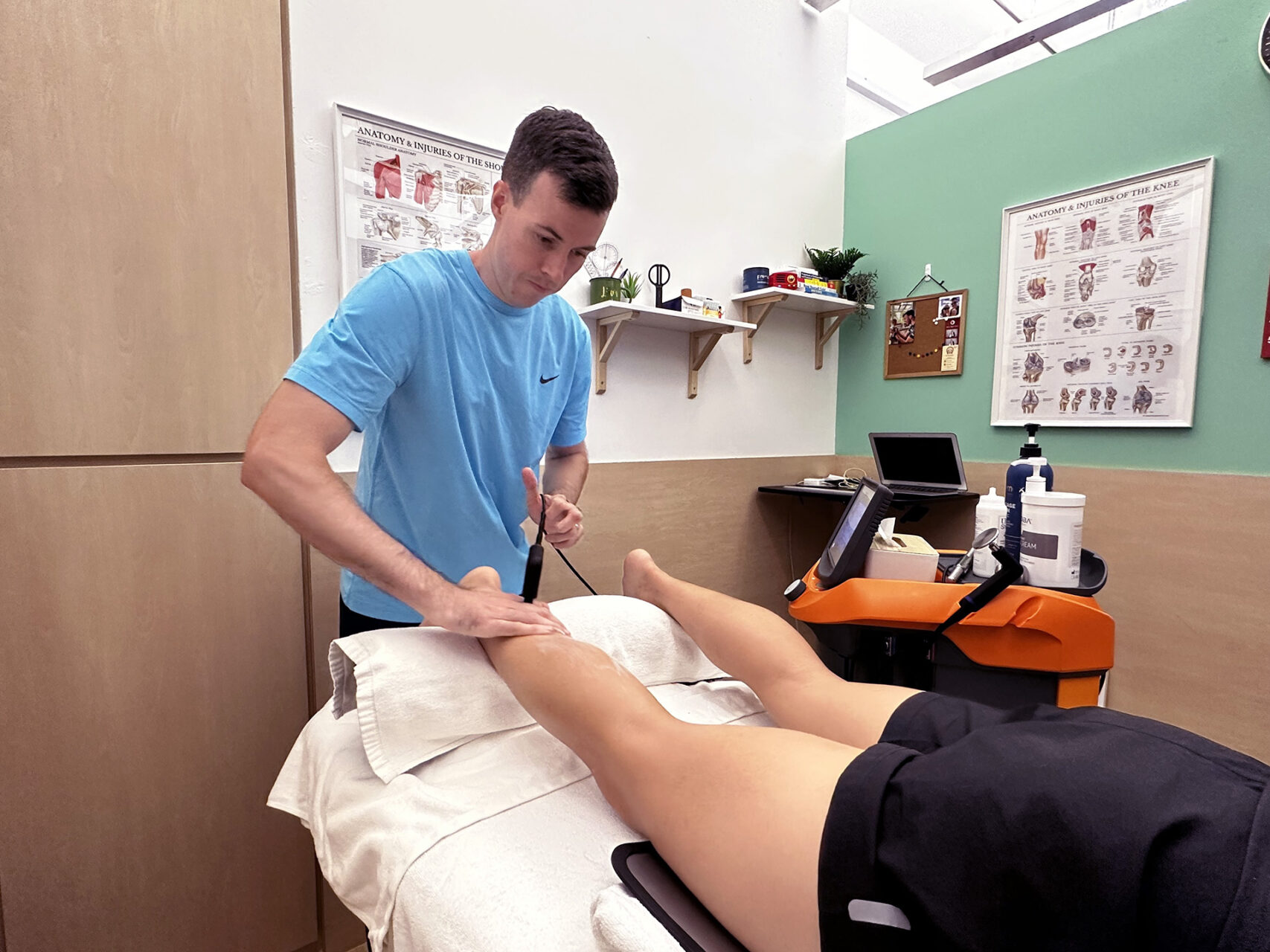
- Shockwave Therapy may be considered for persistent posterior heel discomfort. Focused shockwave is often used when the issue is more localized near the tendon insertion. Radial shockwaves may be used when sensitivity and tightness extend into the calf and surrounding tissues.
- EMTT may be used as a supportive tool for persistent sensitivity and deeper tissue irritation, especially when progress stalls. It is typically paired with a structured strengthening plan rather than used as a stand-alone treatment.
- Retrocalcaneal bursitis taping may help temporarily offload the insertion and improve tolerance during the transition back to activity.
Injections and surgical treatment
If symptoms do not improve with consistent conservative care after a few weeks, a clinician may discuss other options. Surgical treatment is rarely the first step for retrocalcaneal bursitis.
- Corticosteroid injections may be used in selected cases, usually into the retrocalcaneal bursa, often with ultrasound guidance. Injections require careful decision-making around the Achilles tendon in the ankle pain region.
- Retrocalcaneal bursitis surgery is uncommon. Surgical treatment is typically considered only after a thorough non-surgical plan has failed, especially when Haglund’s syndrome or Haglund deformity is contributing to repeated compression of the bursa.
Preventing Retrocalcaneal Bursitis Recurrence
You can help prevent recurrence by making changes to your training and the shoes you wear.
- Maintain calf and ankle flexibility and strength. This is especially important if you run on hills or play sports with a lot of stop-and-start motion (court sports).
- Increase your activity gradually and allow sufficient recovery time between intense workouts.
- Choose footwear that doesn’t put pressure on the posterior area, wear shoes with proper support, and replace worn-out shoes.
- Don’t ignore early signs of discomfort. Rest, reduce your activity, and begin targeted strengthening.
This condition usually results from a combination of factors, including your activity level, ankle movement, calf muscle strength and shoe fit. For the best chance of lasting recovery, address all these areas.
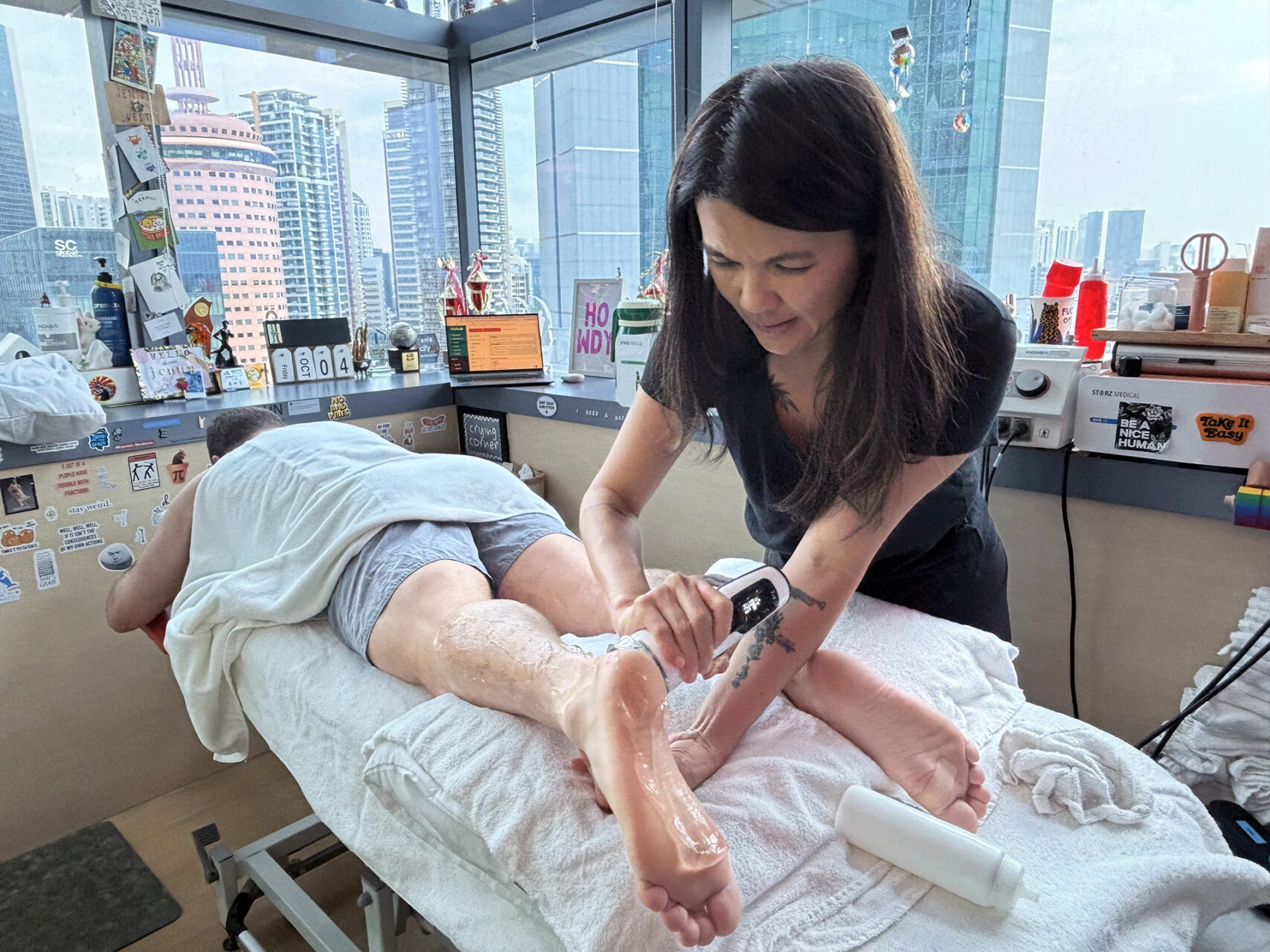
How HelloPhysio Can Help
Heel discomfort limiting activity? Early assessment shortens recovery. At HelloPhysio, our physiotherapists use a physical medicine and physical therapy approach to assess the retrocalcaneal bursa, Achilles tendon, and the mechanics that cause compression. We use hands-on care, exercises, and modalities to help you return to activity with fewer flare-ups. Contact HelloPhysio to book a tailored assessment.

